“Accepting means you allow yourself to feel whatever it is you are feeling at that moment. It is part of the isness of the Now. You can’t argue with what is. Well, you can, but if you do, you suffer.”
~ Eckhart Tolle
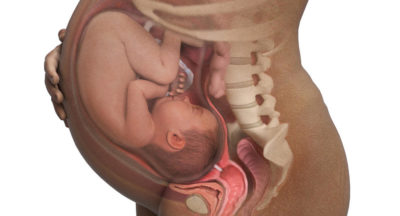
Opioid Dependence, Pregnancy & Breast Feeding
In pregnancy, management of either pain or opioid SUD offers several options. In many cases, medication assisted therapy with either buprenorphine or methadone is advised.
See also:
(Suboxone, Zubsolv, Bunavail, Probuphine)
Key to Links:
Grey text – handout
Red text – another page on this website
Blue text – Journal publication
.
Opioid Dependence, Pregnancy & Breast Feeding
Medication Assisted Treatment (MAT) in Pregnancy
Prior to buprenorphine, treatment options for opioid-dependent pregnant women include medication-assisted withdrawal (i.e., detoxification) and methadone maintenance. Methadone maintenance has previously been the recommended standard of care, preferred over no treatment or medication-assisted withdrawal. Withdrawal from opioids during pregnancy may result in preterm labor, fetal distress, and intrauterine fetal demise.
More recently, buprenorphine has been recommended to treat opioid dependence because findings suggest that buprenorphine treatment during pregnancy has some advantages for infants compared with methadone and is equally safe. Compared with continued opioid abuse, medication assisted treatment during pregnancy lowers risk of developing infectious diseases, including hepatitis and HIV; of experiencing pregnancy complications, including spontaneous abortion and miscarriages; reductions in fetal illicit drug exposure, avoidance of repeated intoxication and withdrawal associated with continued opioid abuse and of having a child with challenges including low birth weight and neurobehavioral problems.
Therapeutic dosing with buprenorphine, as with methadone, avoids the extreme fluctuations in opioid blood concentrations that occur in opioid abuse and place physiological stress on both the mother and the fetus. Compared with methadone, however, buprenorphine may reduce the incidence and/or severity of the neonatal abstinence syndrome (NAS).
Neonatal Abstinence Syndrome (NAS)
When the fetus is exposed to any opioids, including methadone and buprenorphine, the fetus becomes dependent on the medication during pregnancy and typically experiences withdrawal when it separates from the placental circulation at birth. The symptoms of withdrawal, known as neonatal abstinence syndrome (NAS) include hypersensitivity and hyperirritability, tremors, vomiting, respiratory difficulties, poor sleep, and low-grade fevers.
The reported incidence of NAS is highly variable; however, it has been estimated that up to 95% of infants exposed to opioids in utero experience withdrawal and that 50% require treatment. Newborns with NAS often require prolonged hospitalization, during which time they receive medication (usually morphine) in tapering doses to relieve their symptoms while their bodies adapt to becoming opioid-free.
In the definitive “MOTHER” study, it was determined that a child born following buprenorphine treatment exhibits milder NAS symptoms than the one born following methadone treatment. A significant difference in the total amount of morphine administered to neonates treated for NAS between methadone and buprenorphine has been found, with less morphine required to treat NAS in buprenorphine-treated neonates.
The correlation between buprenorphine dose and NAS severity has been inconsistent in the literature. Neonatal urine data suggest that norbuprenorphine, the major buprenorphine metabolite, is predictive of the duration of NAS medication treatment, perhaps because the neonate is delivered with a high concentration of buprenorphine in the blood. Consistent with this reasoning, meconium assays show that total buprenorphine concentrations and buprenorphine/norbuprenorphine ratios are significantly related to the presence of a diagnosable NAS (not necessarily requiring pharmacotherapy.
Finally, it is important to note that the MOTHER study showed that prenatally buprenorphine-exposed neonates had a significantly shorter mean hospital stay and a significantly shorter duration of NAS treatment than did prenatally methadone-exposed neonates. In contrast, the PROMISE study did not find a significant difference between buprenorphine and methadone conditions in neonatal length of hospital stay. Additional research is needed.
Dosing of MAT in Pregnancy
Findings from clinical trials suggest the possible need for buprenorphine and methadone dose increases throughout pregnancy in order to effectively manage withdrawal symptoms in expectant mothers. These findings are consistent with pharmacokinetic research that has shown the need to increase buprenorphine dose during the course of pregnancy in order to maintain therapeutic blood levels. Moreover, These findings are also consistent with past research that has found lowered trough plasma concentrations and greater total and unbound methadone clearances during pregnancy and following delivery in a sample of methadone-maintained pregnant women.
It is estimated that a flexible dose range of 2–32 mg/day of buprenorphine sublingual tablets (monotherapy) is equivalent to a flexible dosing range of 20–140 mg/day of methadone used during pregnancy. Increasing buprenorphine doses beyond 32 mg is not expected to increase the effectiveness of the buprenorphine.
Pain Management: Labor and Delivery and Postpartum
In clinical studies, similar Day 1-5 postpartum pain ratings and pain medication usage were found between methadone- and buprenorphine-maintained women delivering vaginally. Also, following cesarean delivery, women treated daily with either buprenorphine (18 mg) or methadone (80 mg) showed adequate pain control postpartum with the use of a patient-controlled analgesia (PCA) pump for 24 hours, followed by opioids in combination with acetaminophen. Finally, no significant differences were found in pain management between buprenorphine and methadone during delivery or in the immediate postpartum period.
MAT and Fetal Effects
Studies have shown that compared to methadone, buprenorphine produces less suppression of fetal heart rate, fetal heart rate reactivity, and results in a superior biophysical profile after medication dosing. Thus, fetal risk may be no greater, and possibly less, for buprenorphine than for methadone.
Buprenorphine and Neonatal Effects
The definitive PROMISE study reported no physical birth anomalies, with mean values for birth weight, length, and head circumference all exceeding the 50th percentile of WHO standards, and no preterm (<37 weeks) births.
In Conclusion, Methadone versus Buprenorphine
While buprenorphine may be the best option for pregnant women, particularly those who are new to treatment or who become pregnant while on buprenorphine, if a patient is already on methadone maintenance and stable when they become pregnant, she should remain on methadone.
Naloxone in Pregnancy
As a rule, pregnant women are advised to limit fetal exposure to all medications not necessary and not proven safe; thus, prescribing buprenorphine alone avoids fetal exposure to naloxone. Giving naloxone during the fetal stage of organ development to mice and rats at doses up to 6 and 12 times, respectively, the expected human exposure showed no evidence of embryotoxicity or teratogenicity (birth defects). Limited animal studies do suggest that fetal naloxone exposure may produce maternal and therfore fetal hormonal changes, such as increased corticotrophin releasing hormone and adrenocorticotropic hormone. However, there are no studies apparently that evaluate the clinical significance of such hormonal changes and there are no studies in humans that specifically confirm the safety or lack of safety of naloxone in pregnancy.
For these reasons, buprenorphine is most often used as a monotherapy (Subutex) without naloxone during pregnancy.
At some institutions, combination buprenorphine/naloxone are prescribed during pregnancy over the single-entity buprenorphine formulation. The combination product offers the abuse deterrent advantage, namely, the presence of the naloxone limits abuse relapse potential and associated greater safety in reducing relapse exposure to illicit drugs etc. It is believed that because naloxone has poor bioavailability, it should not cause additional concerns during pregnancy compared to single-entity buprenorphine.
While most physicians prescribe monotherapy during pregnancy, there is a lack of consensus regarding the safety trade-off between reduced relapse exposure and potential for an advers outcome associated with fetal hormone changes. It might be argued that monotherapy be prescribed in pregnancy for mothers in extended stable remission whereas the combination buprenorphone/naloxone product be prescribed in higher risk pregnant patients. There are recent studies that appear to confirm the safety of the combination buprenorphine/naloxone in pregnancy. In the case of prescribing the combination product, there may also be an argument to select Bunavail as the drug of choice due to its reported reduced blood levels of norbuprenorphine (see Buprenorphine for SUD or Buprenorphine for Pain) which might in turn reduce the risk of NAS.
MAT and Breast Feeding
Buprenorphine and Breast Milk
Buprenorphine is excreted into breast milk approximately 2 hours after maternal ingestion. Concentrations of buprenorphine and ite major metaboliete, norbuprenorphine, in breast milk are highly variable, due to variations in both milk protein and fat content. However, neither buprenorphine nor norbuprenorphine concentrations were found to exceed blood plasma concentrations. This means that the relative dose per kg of infant body weight is less than 1% of the dose per kg of body weight of the mother and the exposure to the infant of buprenorphine and norbuprenorphine is minimal and considered safe.
Moreover, no known neonatal or child adverse consequences related to exposure to buprenorphine in breast milk have been reported in the literature. Finally, the most recent guidelines recommend breastfeeding for mothers stabilized on either methadone or buprenorphine unless there are clear contraindications (e.g., HIV).
Naloxone in Breast Feeding
Because it is not orally bioavailable, naloxone is unlikely to affect the breastfed infant. Studies in nursing mothers have shown that naloxone does not affect lactation hormone levels. If naloxone is required by the mother, it is not a reason to discontinue breastfeeding.
References:
Addiction – Pregnancy
- Buprenorphine Treatment of Opioid-Dependent Pregnant Women – A Comprehensive Review – 2015
- Neonatal Abstinence Syndrome after Methadone or Buprenorphine Exposure – 2010
- Maternal opioid treatment – human experimental research (MOTHER), approach, issues, and lessons learned – 2012
- Buprenorphine versus methadone in the treatment of pregnant opioid-dependent patients – effects on the neonatal abstinence syndrome – 2005
- Urinary excretion of buprenorphine, norbuprenorphine, buprenorphine-glucuronide, and norbuprenorphine-glucuronide in pregnant women receiving buprenorphine maintenance treatment. – 2009
- Management of Acute Postpartum Pain in Patients Maintained on Methadone or Buprenorphine During Pregnancy – 2009
- Neonatal outcomes following in utero exposure to buprenorphine-naloxone or methadone – 2014
- Buprenorphine + naloxone in the treatment of opioid dependence during pregnancy-initial patient care and outcome data. – PubMed – NCBI
- SUBOXONE & SUBUTEX Patient Information Leaflet
Addiction – Breast Feeding
- ABM Clinical Protocol #21- Guidelines for Breastfeeding and Substance Use or Substance Use Disorder, Revised 2015
- Breastfeeding and Opiate Substitution Therapy – Starting to Understand Infant Feeding Choices – 2016
- Buprenorphine Treatment of Opioid-Dependent Pregnant Women – A Comprehensive Review – 2015
- Buprenorphine and norbuprenorphine concentrations in human breast milk samples determined by liquid chromatography-tandem mass spectrometry. 2005 – PubMed – NCBI
Addiction – Use of Naloxone in Pregnancy
- A comparison of Buprenorphine + naloxone to Buprenorphine and Methadone in the Treatment of Opioid Dependence during pregnancy – Maternal and neonatal Outcomes – 2013
- Endogenous Opioids and Attenuated Hypothalamic–Pituitary–Adrenal Axis Responses to Immune Challenge in Pregnant Rats – 2005
- Reduced activity of the noradrenergic system in the paraventricular nucleus at the end of pregnancy: Implications for stress hyporesponsiveness – 2005
- Naloxone Use During Pregnancy | Drugs.com
- Buprenorphine-naloxone use in pregnancy for treatment of opioid dependence 2016
Neonatal Abstinence Syndrome (NAS) – Overviews
Emphasis on Education
Accurate Clinic promotes patient education as the foundation of it’s medical care. In Dr. Ehlenberger’s integrative approach to patient care, including conventional and complementary and alternative medical (CAM) treatments, he may encourage or provide advice about the use of supplements. However, the specifics of choice of supplement, dosing and duration of treatment should be individualized through discussion with Dr. Ehlenberger. The following information and reference articles are presented to provide the reader with some of the latest research to facilitate evidence-based, informed decisions regarding the use of conventional as well as CAM treatments.
For medical-legal reasons, access to these links is limited to patients enrolled in an Accurate Clinic medical program.
Should you wish more information regarding any of the subjects listed – or not listed – here, please contact Dr. Ehlenberger. He has literally thousands of published articles to share on hundreds of topics associated with pain management, weight loss, nutrition, addiction recovery and emergency medicine. It would take years for you to read them, as it did him.
For more information, please contact Accurate Clinic.
Supplements recommended by Dr. Ehlenberger may be purchased commercially online or at Accurate Clinic.
Please read about our statement regarding the sale of products recommended by Dr. Ehlenberger.
Accurate Supplement Prices
.
