“Be kind whenever possible. It is always possible.”
-14th Dalai Lama
Anxiety & Stress
Anxiety is a mood of fear, worry, and uneasiness resulting from the apprehension of something bad happening, the source of which may or may not be identified. While anxiety can be a normal, appropriate response to circumstances, chronic and irrational or excessive anxiety in response to normal life events can be debilitating and is considered to be an anxiety disorder. In the United States, anxiety disorders effect 40 million adults, representing 15-25% of the population and affecting women 2-3x more often than men.
See also:
Alternative Therapies:
- Animal-Assisted Therapy
- Cognitive Behavior Training (CBT)
- Hypnosis/Self-Hypnosis
- Meditation & Mindful Exercise
- Music Therapy
- Yoga & Tai Chi
Medications:
Complementary and Alternative Medications (CAM):
Nutriceuticals & Supplements:
- Adaptogens
- Ashwagandha
- Bacopa
- Rhodiola Rosea
- Honokiol & Magnolol (Magnolia species)
- Lemon Balm (Melissa officinalis)
- Passion Flower
- Cannabidiol (CBD)
- Magnesium
- Vitamin D
Guided Meditations:
Terence Yallop:
.
Stress
Stress is a general term defined as the nonspecific response of the body to any demand for change and is a normal and natural reaction to a potentially dangerous situation. The stress response is a defensive mechanism that aids in a “fight-or-flight” response to a relevant situation including environmental and psychological conditions. Stress responses are necessary for the survival during a dangerous situation but persistent stress due to environmental or social reasons may trigger health issues including cardiovascular disorders, high blood pressure, depression, panic attacks, impaired memory and cognition, digestive problems, fatigue syndrome and autoimmune disorders. Chronic stress can contribute to genera
lized anxiety disorder (GAD), panic disorder, and obsessive-compulsive disorder (OCD).
Stress is associated with altered hormonal secretions of cortisol, adrenaline, and norepinephrine. Chronic stress disturbs the normal sleep-wake cycle by impacting the level of circadian cortisol. Adaptogens are substances that increase attention and endurance in fatigue, and reduce stress-induced impairments related to the neuro-endocrine and immune systems to improve responses to stress and help the body adapt by normalizing physiological processes. Adaptogens exert their stress-protective effect by regulating the hypothalamic pituitary adrenal (HPA) axis and by controlling key chemical mediators of the stress response. Because stress contributes to the development and maintenance of anxiety, the treatment of anxiety may benefit from stabilizing the individual’s physiologic response to stress through the use of adaptogens.
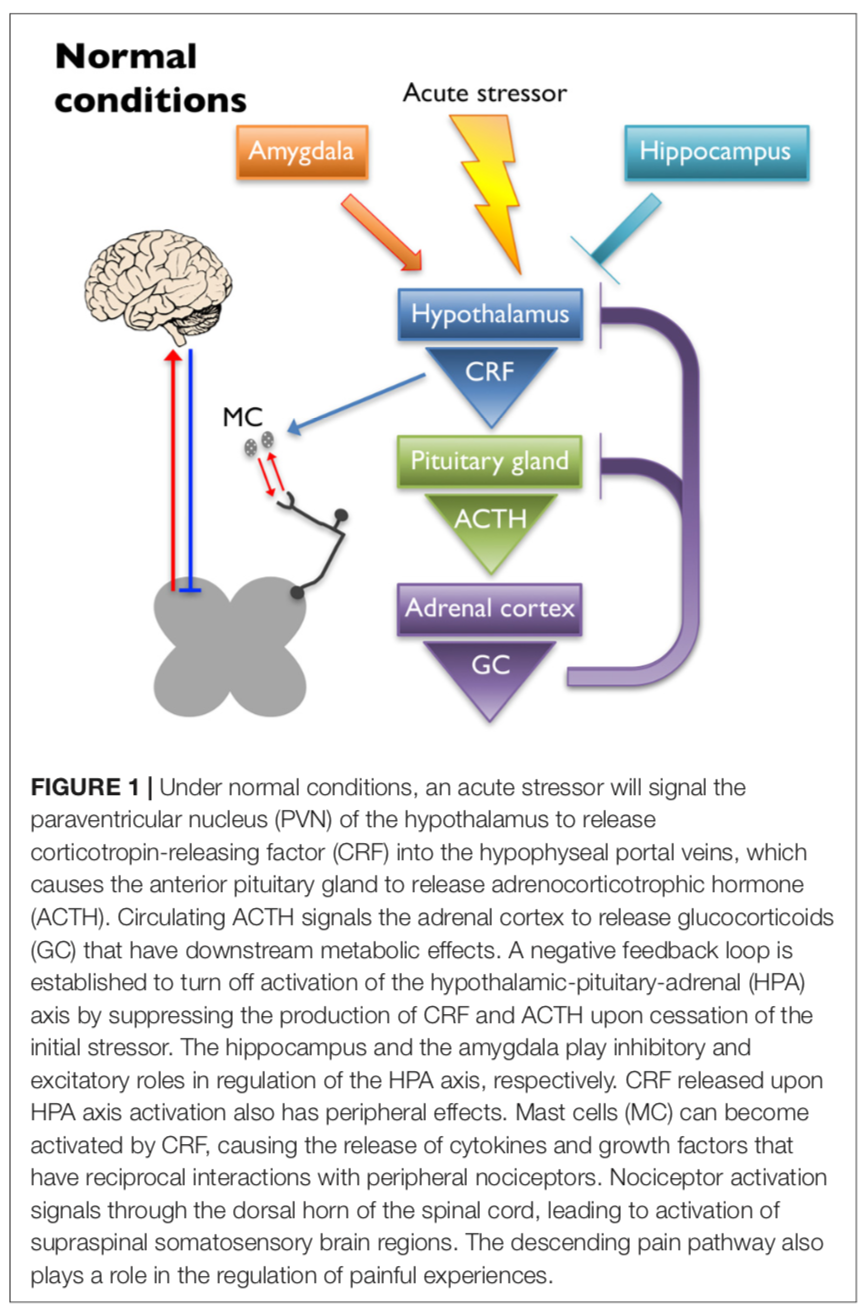
HPA Axis
Taken from: Potential Mechanisms Underlying Centralized Pain and Emerging Therapeutic Interventions – 2018
Anxiety
Anxiety can occur due to a variety of causes. It can be the consequence of medications, dietary deficiency, hormonal changes, illness, traumatic experiences, bad habits and life stressors. Vitamin, mineral and amino acid deficiencies in the diet are associated with increased risk for anxiety disorder. Changes in hormonal balances, particularly associated with women during menstruation, pregnancy, post-partum periods, and menopause are all associated with increased frequencies of anxiety disorder. A traumatic violent experience may lead to post-traumatic stress disorder (PTSD) There may be an inherited genetic basis for anxiety: some studies suggest that variation in neurotransmitter receptor genes are associated with certain forms of anxiety.
Chronic anxiety is associated with greater risk of both cerebrovascular and cardiovascular diseases as well as depression and increased risk of suicide. This relationship with depression can work both ways: anxiety can lead to depression and depression can lead to anxiety. The co-occurrence of anxiety and depression is about 60%. The neurochemistry of anxiety and depression is similar, each sometimes involving imbalances of dopamine and serotonin and both sometimes responding to the same medications.
The Neurochemistry of Anxiety
There is a wide range of neurochemical factors that contribute to anxiety including dysregulation of various neurotransmitters, especially dopamine, norepinephrine and serotonin. Neurotransmitter imbalances in the emotional centers of the brain, the limbic system, as well as dysfunction of the hypothalamic-pituitary-adrenal (HPA) axis are involved. Medical management of anxiety involves modulating these pathways with the use of medications, nutriceutical supplements and behavioral interventions.
Fear, which is often the underlying basis of anxiety, is activated in the amygdala, a key component of the limbic system. Fear results in increased sympathetic nervous activity with subsequent increases in norepinephrine and dysregulation of serotonin balances. These disruptions of serotonin and norepinephrine levels contribute to feelings of anxiety, including physical symptoms. Also, increased activity of the amygdala and hypothalamus increase corticotropic-releasing hormone (CRH), highly implicated in anxiety and depression, which in turn increases cortisol levels. Elevation of CRH is in turn accentuated by elevated serotonin which interferes with the HPA axis’s response to stress. Chronically, this interference leads to high cortisol levels that disrupt circadian rhythm, impair the body’s immune system and ultimately impairs feedback function of the hypothalamus and pituitary which perpetuates anxiety. Anxiety associated with elevated CRH often precedes depression.
Symptoms of Anxiety
Symptoms of anxiety manifest as mental and/or emotional disturbances as well as physical signs and symptoms. It is not unusual for a person to experience only emotional symptoms nor is it unusual for a person to experience physical symptoms and not relate to them as manifestations of their underlying anxiety.
Emotional symptoms include:
- Fear
- Decreased libido
- Decreased emotionality
- Irritability
- Restlessness, inability to relax
- Difficulty concentrating
Physical symptoms include:
- Palpitations
- Difficulty breathing
- Nausea
- Sweating
- Shaking
- Changes in appetite
- Diarrhea
- Dizziness
- Increased pain sensitivity
Types of Anxiety Disorders
There are five main types of anxiety disorder. They are: generalized anxiety disorder (GAD), panic disorder, obsessive compulsive disorder (OCD), phobia and PTSD. In all cases, central nervous system neurotransmitter levels are inappropriate and/or their is imbalance of the Hypothalamic-Pituitary (HPA) axis (which controls noradrenaline and cortisol, the stress hormone).
General Anxiety Disorder
Generalized anxiety disorder (GAD) is characterized by worry in the absence of a real threat or problem. People with GAD are constantly apprehensive and are unable to relax. People with GAD may experience insomnia and fail to concentrate well. A person with mild GAD can manage to keep a career and a social life, however, severe GAD can lead to failure at work and an avoidance of social situations. Women are at a greater risk for GAD than are men and a diagnosis of GAD is made when an individual has three or more of the above symptoms almost daily for six consecutive months.
Panic Disorder
Panic disorder manifests as sudden attacks of fear and a sense of impending doom. This can cause elevated heart rate, sweating, and dizziness. During a panic attack the person may experience shortness of breath, nausea or chest pain. Often these physical symptoms can feedback and make the panic attack worse. Panic attacks are unpredictable, sudden and average 10 minutes duration. Panic disorder affects 6.0 million Americans and is twice as common in women as it is in men.
Obsessive-compulsive disorder (OCD)
Obsessive-compulsive disorder (OCD) is characterized by persistent thoughts (obsessions). The obsessions then cause anxiety and this anxiety leads to the use of ritualistic actions (compulsions) in an attempt to alleviate this anxiety. A good example of OCD is an obsession with bacteria in the environment and a subsequent compulsion to wash hands repeatedly. Approximately 2 million American adults suffer with OCD which affects men and women equally.
Phobias
Phobias are unjustifiable fears. There are specific phobias and social phobias. Specific phobias are a fear of certain agents while social phobia is anxiety about everyday social situations. Social phobia is a chronic fear of being judged by others. A social phobia can last weeks prior to a scheduled encounter or social event. Social phobias affect 15 million Americans.
Posttraumatic Stress Disorder (PTSD)
Posttraumatic stress disorder (PTSD) is initiated by an experience of a traumatic or violent event. This could include a serious accident, a violent crime, or a natural disaster. People with PTSD relive this violent experience in nightmares or wakeful memories. Subsequent ordinary events can trigger “flashbacks” that cause the afflicted person to believe or feel like the event is happening again. Approximately 5 million Americans are affected by PTSD.
Treatment of Anxiety
For the most part, while conventional medicine provides reasonably effective medications for short term managment of anxiety and stress, conventional medicine offers very limited options regarding the treatment of chronic anxiety and stress.
In an attempt to help patients with chronic anxiety and stress, conventional management has tended to “over-medicalize” anxiety and stress. By this it is meant that lifestyle and life circumstance problems are too often treated as medical problems and a medical solution is offered when, in fact, the more appropriate solution lies in lifestyle or cognitive and behavioral solutions rather than the use of medications. As a result of this “over-medicalization,” patients are too often started on medications that have adverse effects, long-term dependency and other problems while at the same time these medications never actually correct the underlying problem.
In truth, while the medical community bears responsibility for the problem of “over-medicalization,” so does western society which seeks a “pill for every ailment,” regardless of the nature of the ailment – medical or not.
The following reviews medical solutions for acute anxiety and stress along with the limited medical options for managing chronic anxiety and stress. At the same time, however, emphasis is placed on behavioral and mind-oriented solutions that have greater effectiveness with better chances of a “cure,” given that there really is no actual “cure,” but instead the cure lies in engaging effective methods for managing the inevitable anxiety and stress that present to all those who are alive.
Conventional Medical Management of Anxiety
Anxiety disorders are treated with conventional “anxiolytic” medicines that fall into four categories:
1.Benzodiazepams including Xanax (alprazolam), Klonapin (clonazepam), Valium (diazepam) and Ativan (lorazepam) work by extending the life of gammaaminobutyric acid (GABA), an inhibitory brain neurotransmitter. GABA is essential to limiting the excitation of neurons and maintain balance.
See: Benzodiazepines
2. Anti-depression drugs, which increase serotonin and dopamine levels, including trazodone, the selective serotonin reuptake inhibitors (SSRI’s) (Prozac, Zoloft, Paxil, Lexapro, and Celexa) and monoamine oxigenase inhibitors (MAOIs) (Nardil,Parnate, Marplan and Emsam) and tricylic antidepressants (TCAs) (Elavil, Doxepin, Desipramine). Selective serotonin reuptake inhibitors (SSRIs) such as Prozac and Paxil reduce amygdala hyper-reactivity to fear-eliciting stimuli. However, SSRI medications are ineffective for many people and may actually aggravate anxiety in some.
3. Azipirone tranquilizers such as buspirone (BuSpar) are prescribed to treat general anxiety disorder (GAD).This class of drug elevates serotonin and dopamine. Buspirone does not have the same tolerance and dependency problems that the benzodiazepines have. Side effects include nausea, headaches, and dizziness.
See: Buspirone (BuSpar)
4. Gabapentinoids [(gabapentin (Neurontin) and pregabalin (Lyrica)] which are used frequently in treating nerve pain are also effective for managing general anxiety as well as benzodiazepine withdrawal-related anxiety.
See: Gabapentin & Lyrica (Gabapentinoids)
5. Beta-blockers (blood pressure medications) which act on the Hypothalamic-Pituitary Axis (HPA) (the connection between the brain and adrenal gland’s release of noradrenaline and cortisol) by blocking the effects of noradrenaline. Beta-blockers include Inderal® (propranolol) and Tenormin® (atenolol) mostly treat the physical symptoms of anxiety such as heart palpitations and sweating. Potential side effects include sexual dysfunction, slow pulse, drowsiness, fatigue, dry mouth, numbness or tingling of fingers or toes, dizziness, diarrhea, nausea, weakness, and cold hands and feet
See: Beta-blockers
Complementary and Alternative Medical (CAM) Management of Anxiety
Medical management of anxiety and stress also includes the use of Complementary and Alternative Medicine (CAM) treatment options, including herbal and natural supplements as adaptogens and anxiolytics. Anxiety, depression, and insomnia are the most common reasons for people to use complementary (CAM) therapies. CAM approaches to the treatment of anxiety include use of nutritional, dietary and herbal supplements, acupuncture, aromatherapy, light therapy, meditation and hypnosis.
See: Meditation and Hypnosis
For the purposes of this section, only dietary, nutritional and herbal supplements and aromatherapy will be reviewed. It should be noted that research evidence for the following CAM treatments are weak due to a lack of large, well-designed studies. While the evidence is encouraging, few agents have strong evidence to recommend their effectiveness. With certain caveats, however, for the most part most of these agents are considered safe with only mild side effects likely. As with all supplements, it is advised that you discuss their use with your physician prior to self-treatment to review safety and dosing precautions.
Diet
Diets high in stimulants have been linked to symptoms of anxiety. Reducing stimulants such as caffeine, chocolate, nicotine and refined sugars will reduce incidence and severity of anxiety. Studies have shown that reduction in dietary fat and alcohol also reduces the vulnerability to stress responses.
Nutritional Supplements
Nutrients and herbs may reduce anxiety by altering both neurotransmitter levels and the HPA axis and have no severe side effects. Vitamins C, D, and E, omega-3 fatty acids, and the green tea amino acid L-theanine increase the production of dopamine. Supplementation with the amino acid L-tryptophan and its precursor, 5-HTP, the B vitamins, vitamin D, selenium, and omega-3 fats increases serotonin production. Amino acid supplements are the nutritional building blocks of neurotransmitter and vitamins act as cofactors in neurotransmitter biosynthesis.
Amino Acids
Various amino acids are proposed to be effective in anxiety, largely related to their role as precursors to the biologic formation of different neurotransmitters including dopamine, serotonin, noradrenaline and GABA, all key players in the neurochemistry of anxiety. The amino acid glutamate is the principle excitatory neurotransmitter and is also used to make the neurotransmitter gamma-aminobutyric (GABA). L-tryptophan and L-tyrosine are precursors for the neurotransmitters, serotonin, dopamine, and norepinephrine. The ability of the body to produce these neurotransmitters is directly linked to the levels of these amino acids consumed in the diet.
L-tryptophan, L-tyrosine and L-phenylalanine
Deficiencies of L-tryptophan, L-tyrosine and L-phenylalanine lead to reduced serotonin production and are associated with anxiety. While the prevalence of these dietary deficiencies is not established in the U.S., supplementing with L-tryptophan is known to increase serotonin synthesis and is often recommended for anxiety and sleep. Supplementing with 5-hydroxytryptophan (5-HTP), the tryptophan precursor, and tryptophan have been shown to elevate brain serotonin levels and enhance a sense of well-being.
Supplementing with D,L-phe
nylalanin
e and L-tyrosine increases synthesis of dopamine and norepinephrine supporting their role in fighting anxiety. D,L-phenylalanine is also recommended in opioid withdrawal and may have a role in reducing chronic pain.
L-theanine
L-theanine, an amino acid found in tea (Camellia sinensis), has been shown in several studies to increase dopamine and serotonin production and GABA activity, resulting in a relaxed yet alert state.
A daily dose of L-theanine of 200-400 mg has been recommended
Minerals
Magnesium
In a placebo controlled clinical study, when magnesium was taken orally along with calcium supplements, anxiety was decreased compared to placebo. Similarly, supplementation with magnesium and vitamin B6 was shown to reduces premenstrual-related anxiety and GAD in women. Magnesium supplementation has also been found to be effective in many conditions often associated with anxiety including chronic muscle pain/spasm, migraine headaches and insomnia.
It should be noted that the absorption of magnesium may be superior when absorbed through the skin through the use of epsom salt baths as well as less side effect of diarrhea, commonly seen with oral use supplementation with magnesium. It has been reported that dietary insufficiency of magnesium is common in the U.S., with estimates as high as 80% prevalence in women and 70% in men. The argument for epsom baths 3-4x/week for patients with chronic pain and anxiety is particularly high when factoring in the benefit of 15-20 minutes of “off-time” with a quiet soak.
See: Magnesium
Selenium
In clinical trials people given daily oral supplementations of 100 mg of selenium for 5 weeks reported less anxiety. Confirmatory research is lacking as to cause-effect and to prevalence of selenium deficiency as a contributor to anxiety.
Fatty acids
Omega-3 fatty acids
Dietary supplementation with omega-3 fatty acids has been shown to both improve mood and reduce the risk of anxiety. Again, studies are lacking to confirm these benefits for anxiety, but omega-3 fatty acids are also thought to have beneficial roles in cardiovascular health and oxidative stress. That being said, it is likely that the best approach here would be to include fish in one’s diet with at least 5 servings/week to maintain adequate nutritional quality and balance of the omega-3 fatty acids.
Vitamins
Because Vitamin C is a cofactor for enzymes involved in biosynthesis, and it is effective for oxidative stress and possibly reducing levels of stress-related cortisol, supplementation with Vitamin C to reduce anxiety has been advocated by some. One clinical study did show that high dose vitamin C improves mood, but substantial research for this anxiolytic benefit is lacking. Vitamin E also may reduce anxiety and vitamin D supplementation may reduce anxiety in patients with fibromyalgia-associated anxiety.
See: Vitamin D
Herbs and Botanicals for Anxiety
Ashwagandha
Ashwagandha (Withania somnifera (L.) Dunal) is a plant found in Asia and has been used in traditional Ayurveda (Hindu) medicine for literally thousands of years. It has been shown to reduce anxiety, improve sleep and fatigue and reduce the impact of stress. Pharmacological studies have demonstrated that Ashwagandha may have anti-inflammatory, neuroprotective, and memory-enhancing properties.
See: Ashwagandha
Cannabidiol (CBD)
Cannabidiol (CBD) is one of the major constituents found in marijuana, second in abundance in the plant only to THC. Unlike THC, which provides the euphoria and “high” associated with the use of marijuana, CBD does not cause any euphoria or “high” and does not impair thought processing aside from its potential for sedation as a side effect in some people, and with high doses. Since CBD has become legal in the U.S. and is now available as an affordable over-the-counter medication, it has been found to have proven benefits in the management of anxiety as well as insomnia.
CBD’s benefit for anxiety has been studied in humans since 1982 and has shown to be safe with few side effects, mostly limited to sedation. CBD is effective for general anxiety (GAD), panic disorder, post-traumatic stress disorder (PTSD) and social anxiety (SAD). In most early studies an oral dose of CBD between 300-600 mg/day was employed and was well-tolerated in doses up to 1,500 mg/day. Subsequently it has been shown to effective at doses as low as 25-100mg/day. As with most medications, dosing should be initiated at low doses and gradually increased as needed to achieve the desired response and avoid side effects. Recent research suggest CBD has a biphasic dosing response, meaning that sometimes lower doses are more effective than higher doses. CBD is available in liquid form, powders and capsules.
See Cannabidiol (CBD) – Clinical Use and Dosing)
Kava Kava (Piper methysticum)
The best studied botanical with the most established benefit is kava kava (Piper methysticum). Unfortunately, recommendations for its use have been clouded by controversial concerns regarding its safety with respect to liver toxicity. The controversy is based on rare reports of liver toxicity, but apparently the only reported cases of this liver toxicity stemmed from the use of extracts from kava that included not just the kava root that is the traditional source for use, but also extracts from the stems and leaves. It is believed that the solvents and/or the extraction process is what lead to the few reported cases rather than traditional use of simple water extracts from the kava root. As a result of these insights, kava once banned in Canada and the United Kingdom is now again available. It has never been banned in the U.S.
There are six psychoactive agents in kava, kavalactones, and they bind to GABA receptors, dopamine receptors and opiate receptors and they also uncouple sodium potassium channels thereby reducing impulses to muscles causing muscle relaxation. The anxiolytic benefits of Kava have been compared to the use of benzodiazepines. It may also be effective for symptoms of premenstrual syndrome.
GABA
GABA is an inhibitory neurotransmitter of the central nervous system that reduces nerve impulse transmission between neurons (through the hyperpolarization of postsynaptic membranes and the reduction of neurotransmitter release into the synapse through presynaptic G-protein coupled receptor inhibition of voltage-gated Ca++ mechanisms). GABA is also found occurring naturally in herbs and plants and it works by reducing the excitability of a neural network thereby functioning as a brake on the neural circuitry during stress. Low GABA levels are associated with restlessness, anxiety, insomnia and a poor mood state. Dietary GABA supplement has been shown in some clinical studies to relieve anxiety.
Honokiol
Honokiol, found in Magnolia bark (Magnolia officinalis), is one of the most important traditional herbal medicines in China and Japan used to treat clinical depression and anxiety-related disorders and has been in use for 1000 years. The oldest known traditional Chinese medicine book, Shennong Bencao Jing, mentions this tranquilizing action. M. officinalis is prescribed for clinical depression, anxiety-related disorders and insomnia. Honokiol is also known to benefit pain, especially neuropathic pain.
See: Honokiol.
Honokiol reduces anxiety at low doses (100-400 mg). This benefit is believed to be partially attributed to its interaction with GABA-A receptors, the same target as benzodiazepines (such as Valium (diazepam) and other anxiolytics. Honokiol may also alter the brain’s synthesis of GABA, an inhibitory neurotransmitter in the brain.
Honokiol is commercially available in combination with PEA, a neuropathic pain agent, in a product called ComfortMax.
Lavender (Lavender angustifolia)
The anxiolytic benefits of the volatile oil of lavender has been demonstrated in many randomized clinical trials. One study compared an oral lavender extract (Silexan) to lorazepam (Ativan) for the treatment of general anxiety and found that 40% of the lavender group went into remission compared to 27% of the lorazepam group. Lavender has also been evaluated as an aromatherapy and has been shown to be beneficial by nasal inhalation as well.
Linalool, a terpene, is the most abundant constituent found in lavender and is thought to contribute to both the characteristic aroma of lavender as well as its therapeutic benefits for anxiety and sleep. Interestingly, linalool is also one of the most abundant terpenes found in most cannabis (marijuana) strains (see Terpenes, an Overview). It has been found that the marijuana strains with the most linalool are the strains that also are best known for their relaxing effects and benefits for reducing anxiety. Lavender oil improves sleep efficiency, increases total sleep time, improves energy the following morning and promotes sleep in patients with insomnia.
Linalyl acetate, the other primary terpenoid in lavender, is broken down to linalool in the stomach which also contributes to the anxiolytic benefits of oral use of lavender extracts. The mechanism of action of linalool for its sedative, anxiolytic and anticonvulsant properties is likely the modulation of glutamate and GABA neurotransmitter systems.
Oral intake of linalool, in the form of lavender essential oil (Silexan™) capsules wa demonstrated to be effective for anxiety in a meta-analysis published in 2019. Five studies with a total of 524 participants received treatment with Silexan™ 80 mg and 121 participants taking silexan 160 mg. Silexan™ 80 mg was observed to be effective for anxiety, equivalent to that of paroxetine (Paxil), a prescription SSRI (selective serotonin reuptake inhibitor). Overall, Silexan™ 160 mg was found to be more effiective than Silexan™ 80 mg. Silexan™ contains primarily linalool (36.8%) and linalyl acetate (34.2%). Minor components of Silexan™ include monoterpene alcohol lavandulol, its ester lavandulyl acetate, and bicyclic monoterpenoids borneol, eucalyptol (1,8-cineole) and camphor.
OTC Products
Lavender oil is available in a number of over-the-counter (OTC) medications directed at treating anxiety and to promote relaxation and calm. As noted above, Silexan™ is a formulation of lavender oil that has been studied and found to be effective for these conditions and can used to supplement marijuana products. Although Silexan™ does not seem to be available directly, it is found in different brands of OTC meds, such as Nature’s Way “CalmAid®” in 80mg softgels to be dosed at 80-160 mg/day. Other OTC products similarly available list “lavender oil,” 80mg) but not specifically as Silexan™ and may provide identical benefits,
Lemon balm (Melissa officinalis)
Based on a recent literature review, it was concluded that extracts of M. officinalis are effective in reducing anxiety and stress due to its action on the central nervous system, particularly the cholinergic and GABAergic systems, though its exact mechanism of action is still controversial.
< span style=”color: #808080;”>
The GABA-A receptors are ionic channels that mediate the effects of GABA, producing an inhibitory action through the opening of chloride channels preventing a neuronal action potential. This is seen as the mechanism of action of diazepam (Valium) and is believed to be one of the possible mechanisms of action of Lemon Balm.
Lemon Balm is widely used with another plant, Valerian (Valeriana officinalis), for relieving sleep difficulties, tension, restlessness, and irritability.
Passion Flower
Multiple animal and human studies performed over the last ten years have demonstrated the effectiveness of Passion Flower extract for anxiety comparable to benzodiazepines. Compared to the benzodiazepines, Passion Flower may not have as rapid onset, but it appears to be less likely to impair memory and no withdrawal syndromes from Passion Flower have been reported.
See Passion Flower
Valerian (Valeriana officinalis)
Valerian is a temperate plant root that has been used medicinally since the time of Hippocrates as a remedy for sleep and anxiety. It has been shown to be effective as a hypnotic (sleep agent), with particular effectiveness for benzodiazepine withdrawal-related insomnia, suggesting that it is likely to also be effective for benzodiazepine withdrawal-related anxiety.
Valerian root components have been shown to both increase GABA synthesis and decrease synaptic GABA reuptake. Valerian root activates glutamic acid decarboxylase, an enzyme involved in the synthesis of GABA. The active Valerian root extract known as valernic acid acts as a GABA agonist by binding to GABA receptors. Valerian root extracts have anxiolytic properties at doses of 400–900 mg daily. Valerian root has been shown in some research to be as effective as diazepam in reducing anxiety. More research is needed to confirm these findings but Valerian root has established safety profiles that would argue for an initial trial of Valerian root for anxiety before starting benzodiazepines.
Anxiety and Hormones
Anxiety disorders in general affect more women than men. Furthermore, pregnant, postpartum, premenstrual and menopausal women also experience symptoms of anxiety to a greater extent than at other times in life. This general observation has lead researchers to investigate a link between hormones and anxiety. By now, it is well known that most steroid sex hormones (e.g., pregnenolone, estrogen, progesterone, testosterone, and DHEA – a precuror to building the sex hormones) are neurologically active. In fact, the brain has large quantities of DHEA along with estrogen and progesterone receptors. These hormones have a number of effects within the brain, including regulation of mood.
A number of studies have linked abnormalities in hormone levels to various anxiety disorders. During the first week of menses when there are increased levels of estrogen, women produce more serotonin and have improved mood. Decreased estrogen and serotonin levels are associated with the premenstrual period when there is often impaired mood and increased anxiety. In addition, the drop in estrogen during menopause is associated with reduced serotonin production and more anxiety. It has been shown that the selective serotonin reuptake inhibitors (SSRIs) used to treat anxiety have also been shown to improve mood and cognitive function in menopausal women.
DHEA
During times of prolonged stress a greater proportion of cortisol (the stress hormone) is made compared to DHEA such that increased blood cortisol/DHEA ratios are believed to be a marker of stress and are associated with anxiety disorder. Women with insufficient progesterone levels are more susceptible to anxiety and studies indicate supplementing these women with proegesterone, or DHEA, can reduce anxiety.
Cordoncillo (Piper hispidum)
Recent research has looked at a Central American plant (Piper hispidum) that has been traditionally used by Q’eqchi Maya healers, midwives, and community members in Guatemala for female reproductive disorders. The leaves of Piper hispidum are used to prepare a tea for the treatment of amenorrhea (lack of menses), dysmenorrhea (abnormal menses), menopause and pain and are considered effective.
Researchers have found that that extracts of the leaves of Piper hispidum (butenolides) bind to both the estrogen receptor and serotonin receptors and act as serotonin and estrogen agonists, thus explaining the mechanism of benefit for these disorders and suggesting a possible use for anxiety related to menstrual complaints. No evidence was found for drug interactions related to inhibition of CYP450 liver enzymes. More research is needed.
Commercial Products for Anxiety
Without intending to specifically promote any individual commercial product, based on anecdotal reports from patients with positive results some products are presented here as offering potential benefit for anxiety and stress management. An effort has been made to confirm the safety and effectiveness of the product and/or its ingredients prior to listing the product here.
Opidone
Opidone is promoted as an effective supplement for anxiety and stress. While there is some evidence for the effectiveness of the individual substances making up Opidone’s formula which suggests the product may be helpful, no studies evaluating this specific product appears to be available.
See: Opidone
The individual substances making up the Opidone formula include:
(1) PharmaGaba
(2) Agmatine
(3) L-Theanine
(4) Magnolia Bark Extract (contains the active ingredients Honokiol and Magnolol)
(5) Ginger Root
RediCalm
RediCalm is also promoted as an effective supplement for anxiety and stress. While there is some evidence for the effectiveness of the individual substances making up RediCalm’s formula which suggests the product may be helpful, no studies evaluating this specific product appears to be available.
See: RediCalm
The individual substances making up the RediCalm formula include:
(1) Ashwaganda
(2) Passion Flower
(3) L-Theanine
(4) Lemon Balm
(5) 5-HTP
Behavioral Management of Anxiety
Bebavioral management of anxiety and stress includes Cognitive Behavioral Training (CBT), meditation, hypnosis, yoga and other “mindful exercises,” even listening to muic, that are actually very effective and easily learned and engaged into dail practice. All of these modalities are offered at Accurate Clinic to those interested in pursuing them. While they all require greater commitment than simply swallowing a pill, these options are very effective with their outcome and benefits proportional to the effort placed in engaging them.
See: CBT, Meditation and Music Therapy, Hypnosis and Yoga
This page remains unfinished: an overview and summary of the articles below is forthcoming. In the meantime, please review the articles below.
Resources:
Benzo.org.uk is the best resource for learning about discontinuing benzodiazepines:
References:
Anxiety & Stress – Overviews
Anxiety & Stress – Prescription Medications
Anxiety & Stress – Benzodiazepines
Anxiety & Stress – Buspirone: MedlinePlus Drug Information.pdf (Buspar)
Anxiety & Stress – Gabapentinoids: (Lrica (pregabalin) & Neurontin (gabapentin)
Anxiety – Lyrica
- Pregabalin in acute treatment of anxious depression – 2013
- Pregabalin in Generalized Anxiety Disorder – A Placebo-Controlled Trial – 2003
- The treatment of generalized anxiety disorder with pregabalin, an atypical anxiolytic – 2007
- Efficacy of pregabalin in the treatment of generalized anxiety disorder: double-blind, placebo-controlled comparison of BID versus TID dosing. – PubMed – NCBI no higlights
- Pregabalin – A guide to its use in fibromyalgia, neuropathic pain and generalized anxiety disorder – 2014
Anxiety – Gabapentin
Anxiety & Stress – SNRIs (Selective Norepinephrine and Serotonin Reuptake Inhibitors)
Anxiety & Stress – SSRIs (Selective Serotonin Reuptake Inhibitors)
Anxiety & Stress – Exercise
Anxiety & Stress – CAM Treatment
Anxiety & Stress, CAM Tx – Overviews
- What Can CAM Do for Anxiety?
- Complementary and alternative medicine in the treatment of anxiety and depression – 2008
- Natural Medicine Treatment Considerations for Generalized Anxiety Disorder – 2014
Anxiety & Stress, CAM Tx – Natural, Herbal Options Overviews
- Dietary_and_botanical_anxiolytics – 2012
- Natural Nutritional Supplements for Anxiety and Depression Treatment
- Herbal remedies for anxiety – a systematic review of controlled clinical trials. – PubMed – NCBI
- [Medicinal plants for the treatment of generalized anxiety disorder: a review of controlled clinical studies]. – PubMed – NCBI
- Plant-Based Medicines for Anxiety Disorders, Part 1 – A Review of Preclinical Studies – 2013
- Plant-Based Medicines for Anxiety Disorders, Part 2 – A Review of Clinical Studies with Supporting Preclinical Evidence. – PubMed – NCBI
- Complementary and alternative medicine in the treatment of anxiety and depression – 2008
Anxiety & Stress, CAM Tx – Ashwaganda (Withania somnifera)
- An Alternative Treatment for Anxiety – A Systematic Review of Human Trial Results Reported for the Ayurvedic Herb Ashwagandha (Withania somnifera) – 2014
- Naturopathic Care for Anxiety – A Randomized Controlled Trial – 2009
Anxiety & Stress, CAM Tx – Lavender, Overviews
- An Orally Administered Lavandula Oil Preparation (Silexan) for Anxiety Disorder and Related Conditions- An Evidence Based Review – 2013
- Lavender and the Nervous System – 2013
- In-vitro inhibition of human erythrocyte acetylcholinesterase by salvia lavandulaefolia essential oil and constituent terpenes. – PubMed – NCBI – 2000
- A question of scent – lavender aroma promotes interpersonal trust – 2015
Anxiety & Stress, CAM Tx – Lavender, Anxiety
- Essential oil of lavender in anxiety disorders – Ready for prime time? – 2017
- The Effect of Lavender Aroma on Anxiety of Patients Having Bone Marrow Biopsy- 2020
Anxiety & Stress, CAM Tx – Lavender, Anxiety – Silexan
- A Multi-Center, Double-Blind, Randomised Study of the Lavender Oil Preparation Silexan in Comparison to Lorazepam for Generalized Anxiety Disorder – 2010
- Is Lavender an Anxiolytic Drug? A Systematic Review of Randomised Clinical Trials – 2012
- An Orally Administered Lavandula Oil Preparation (Silexan) for Anxiety Disorder and Related Conditions- An Evidence Based Review – 2013
- Lavender oil preparation Silexan is effective in generalized anxiety disorder – a randomized, double-blind comparison to placebo and paroxetine – 2014
- Silexan in anxiety disorders – Clinical data and pharmacological background – 2017
- Silexan in anxiety disorders Clinical data and pharmacological background – PubMed – 2018
- Efficacy and safety of lavender essential oil (Silexan) capsules among patients suffering from anxiety disorders – A network meta-analysis – 2019
- Efficacy of Silexan in subthreshold anxiety – meta-analysis of randomised, placebo-controlled trials – 2019
- Therapeutic effects of Silexan on somatic symptoms and physical health in patients with anxiety disorders – A meta- analysis – 2020
Anxiety & Stress, CAM Tx – Lavender, Sleep
- An olfactory stimulus modifies nighttime sleep in young men and women. – PubMed – NCBI
- Lavender and sleep – A systematic review of the evidence – 2012
- Effects of odorant administration on objective and subjective measures of sleep quality, post-sleep mood and alertness, and cognitive performance – 2003
- Odors enhance slow-wave activity in non-rapid eye movement sleep – 2016
- Effectiveness of Silexan Oral Lavender Essential Oil Compared to Inhaled Lavender Essential Oil Aromatherapy for Sleep in Adults- A Systematic Reviewv – 2018
Anxiety & Stress, CAM Tx – Lemon Balm (Melissa Officinalis)
- Anxiolytic properties of Melissa officinalis and associated mechanisms of action – A review of the literature – 2015
- modulation-of-mood-and-cognitive-performance-following-acute-administration-of-single-doses-of-melissa-officinalis-lemon-balm-2002
- melissa-officinalis-l-a-review-of-its-traditional-uses-phytochemistry-and-pharmacology-pubmed-ncbi
- Lemon balm | University of Maryland Medical Center
Anxiety & Stress, CAM Tx – Passion Flower
- Passiflora incarnata L. Improves Spatial Memory, Reduces Stress, and Affects Neurotransmission in Rats. – PubMed – NCBI
- Passiflora incarnata L. (Passionflower) extracts elicit GABA currents in hippocampal neurons in vitro, and show anxiogenic and anticonvulsant effects – 2010
Anxiety & Stress, CAM Tx – Yoga
- Yoga for the primary prevention of cardiovascular disease. – PubMed – NCBI
- iRest Yoga-Nidra on the College Campus – Changes in Stress, Depression, Worry, and Mindfulness
- Individualized yoga for reducing depression and anxiety, and improving well-being: A randomized controlled trial
- Yoga Practice Associations with Mindfulness, Kundalini, and Mystical Experiences – 2015
- Yoga as an Adjunctive Treatment for Posttraumatic Stress Disorder – A Randomized Controlled Trial – 2014
- The Effects of a Hatha Yoga Intervention on Facets of Distress Tolerance – 2015
- Recent Development in Yoga – A Scientific Perspective – 2016
Anxiety & Stress, CAM Tx – Music Therapy
- Music listening as a means of stress reduction in daily life. – PubMed – NCBI
- The impact of acute stress on hormones and cytokines and how their recovery is affected by music-evoked positive mood – 2016
.
Emphasis on Edu
cation
Accurate Clinic promotes patient education as the foundation of it’s medical care. In Dr. Ehlenberger’s integrative approach to patient care, including conventional and complementary and alternative medical (CAM) treatments, he may encourage or provide advice about the use of supplements. However, the specifics of choice of supplement, dosing and duration of treatment should be individualized through discussion with Dr. Ehlenberger. The following information and reference articles are presented to provide the reader with some of the latest research to facilitate evidence-based, informed decisions regarding the use of conventional as well as CAM treatments.
For medical-legal reasons, access to these links is limited to patients enrolled in an Accurate Clinic medical program.
Should you wish more information regarding any of the subjects listed – or not listed – here, please contact Dr. Ehlenberger. He has literally thousands of published articles to share on hundreds of topics associated with pain management, weight loss, nutrition, addiction recovery and emergency medicine. It would take years for you to read them, as it did him.
For more information, please contact Accurate Clinic.
Supplements recommended by Dr. Ehlenberger may be purchased commercially online or at Accurate Clinic.
Please read about our statement regarding the sale of products recommended by Dr. Ehlenberger.
Accurate Supplement Prices
.