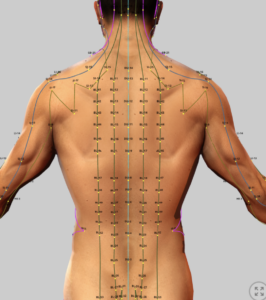
Acupuncture:
Trigger Points and Myofascial Pain
Acupuncture involves the insertion of thin needles into specific points along the meridians to stmulate the flow of Qi and alleviate pain and other conditions.
See:
- Trigger Point Therapy
- Myofascial Pain
- Trigger Points & Acupuncture Points
- Acupressure Massage
- See:
- Traditional Chinese Medicine (TCM)
- TCM – Chinese Herbal Medicine (introduction)
- Acupuncture – Introduction
- Acupuncture – Migraine Headaches
- Acupuncture – Trigger Point & Myofascial Pain
- Acupuncture – Osteoarthritis
- Acupuncture – Peripheral Neuropathy (Overview)
- Acupuncture – Diabetic Peripheral Neuropathy (DPN)
- Acupuncture – Chemotherapy-Induced Peripheral Neuropathy (CIPN)
- Acupuncture – Sciatica
- Acupuncture – Fibromyalgia
- Acupuncture – Mechanisms of Actions
- Acupuncture – Transition from Acute to Chronic Pain
Nutraceuticals:
This Page:
Acupuncture
Integration with Modern Healthcare:
Traditional Chinese medicine (TCM) is a system of medicine that has been practiced for thousands of years and is gaining popularity in the West. In fact, even in modern China that is experiencing more and more influence from the west in terms of medicine, food and lifestyle, the use of TCM including acupuncture is growing in popularity over the last decade, not receiving as one might have predicted. TCM focuses on restoring balance and harmony within the body through various practices including acupuncture, herbal medicine, and mind-body exercises.
Acupuncture is commonly used effectively for a wide range of conditions, such as pain, musculoskeletal disorders and several neurologic diseases Acupuncture treatment is based on the Chinese theory that illness results from imbalances in energy flow, or qi, and fine acupuncture needles are inserted at specific points on the body to correct these imbalances and restore harmony. Western science has proposed different theories as to how acupuncture works, including teh Gate Control theory and the release of endogenous opioids, but none of the theories appear to be fully satisfactory and acupuncture remains largely not well understood.
Acupuncture is generally considered safe when performed by a certified practitioner. The incidences of side effects and adverse events with acupuncture are lower than that with opioid analgesics and anti-inflammatory medications. Studies have shown it to be effective for pain relief, managing chemotherapy side effects, and improving quality of life. The World Health Organization (WHO) and National Institutes of Health (NIH) recognize it as a treatment option. While promising research exists, further high-quality studies are needed to fully understand its efficacy and mechanisms.
- Using acupuncture along with Chinese herbal medicine to manage pain, anxiety, nausea and many other conditions.
- Incorporating TCM practices like tai chi and meditation for stress and mental health support.
Acupuncture Management: Trigger Points and Myofascial Pain
At Accurate Clinic and most pain management programs, the most common source of chronic pain is myofascial pain syndrome (MPS), including (trigger points and localized muscle pain). MPS frequently accompanies chronic spine pain of the neck and back related to their arthritis and/or disc problems. Myofascial pain also frequently accompanies joint pain, especially the shoulder muscles that elevate and move the shoulder .
This section reviews findings from high quality research (Cochrane reviews, systematic reviews, and meta-analyses) published between 2020 and 2025) that evaluates acupuncture for myofascial pain.
Myofascial Pain (trigger points and muscle pain)
Effectiveness:
- Acupuncture is effective for myofascial pain syndrome, particularly for short-term pain relief and improved function. Recent systematic reviews and meta-analyses (2020–2025) demonstrate moderate to high-quality evidence supporting its use, especially for chronic myofascial pain in regions like the neck, shoulders, and low back.
Key Studies:
- A 2020 systematic review and meta-analysis (Fernández-de-las-Peñas et al.) analyzed 15 Random Controlled Trials (RCTs) (1,263 subjects) and found acupuncture significantly reduced pain intensity compared to sham acupuncture and no treatment for myofascial pain. Benefits were most pronounced at 4–12 weeks post-treatment.
- A 2022 meta-analysis (Li et al.) of 20 RCTs (1,892 subjects) confirmed acupuncture’s effectiveness for myofascial trigger point pain, with a significant reduction in pain scores compared to sham and active controls (e.g., physical therapy). Dry needling, a form of acupuncture targeting trigger points, showed similar efficacy.
- A 2024 systematic review (Zhang et al.) included 12 RCTs focusing on myofascial pain in the neck and shoulder, concluding that acupuncture (manual and electroacupuncture) improved pain and range of motion compared to sham, with effects lasting up to 3 months.
- No Cochrane reviews specifically address myofascial pain alone, but a 2020 Cochrane update on acupuncture for chronic pain (including myofascial pain) supports moderate-quality evidence for pain relief and functional improvement.
Specific Findings:
- Acupuncture is particularly effective for myofascial pain associated with neck and shoulder trigger points, with evidence suggesting superiority over sham for pain reduction and muscle relaxation.
- Electroacupuncture may enhance outcomes compared to manual acupuncture, especially for severe trigger point pain, due to stronger stimulation of muscle fibers.
- Compared to other treatments (e.g., NSAIDs, physical therapy), acupuncture shows comparable or superior short-term pain relief with fewer side effects, though long-term benefits (>6 months) are less clear.
Dosing and Scheduling
- Protocols: Most studies recommend 6–12 sessions, 20–30 minutes each, over 4–8 weeks, with 1–2 sessions per week. Electroacupuncture protocols may use slightly fewer sessions (4–8) due to intensified stimulation.
- Trigger Point Focus: Acupuncture often targets myofascial trigger points directly (e.g., ashi points) or combines local points with distal points (e.g., LI4, ST36) based on TCM or Western medical acupuncture (WMA) principles.
- Maintenance: Some studies suggest maintenance sessions every 1–2 months for chronic myofascial pain to sustain benefits, though evidence for optimal maintenance is limited.
Mechanism of Action
- Proposed Western Neurophysiological Mechanisms:
- Acupuncture stimulates sensory nerves at trigger points, modulating pain via the gate control theory and descending inhibitory pathways.
- Triggers release of endogenous opioids (e.g., endorphins) and modulates neurotransmitters like serotonin and norepinephrine.
- Reduces local muscle tension and ischemia in trigger points, improving blood flow and oxygenation.
- TCM Perspective: Acupuncture is thought to restore qi flow and resolve stagnation in meridians, though this is less emphasized in modern research.
- Electroacupuncture: Enhances effects by stimulating muscle fibers, potentially disrupting taut bands in trigger points and promoting muscle relaxation.
Safety
- Adverse Events: Acupuncture is safe with a low risk of serious adverse events. Common side effects include:
- Minor pain or soreness at needle sites (~30–48% of trials).
- Bruising or bleeding (~10–20%).
- Transient dizziness or fatigue (~5–10%).
- Serious Risks: Rare (e.g., pneumothorax, infection), occurring in <0.01% of cases when performed by trained practitioners using sterile needles.
- Comparison: Acupuncture has fewer side effects than pharmacological treatments (e.g., NSAIDs, muscle relaxants) commonly used for myofascial pain.
Cost
- Range: $50–$150 per session in the U.S., depending on location, practitioner expertise, and session length.
- Insurance Coverage: Variable, with some plans covering acupuncture for chronic pain (e.g., Medicare for chronic low back pain since 2020). Coverage for myofascial pain specifically is less common, often requiring out-of-pocket payment.
- Cost-Effectiveness: Limited data, but a 2021 study suggested acupuncture may be cost-effective for chronic pain when compared to long-term NSAID use, given reduced medication-related adverse events.
Evidence Quality
- Overall Quality: Moderate to high for short-term pain relief and functional improvement in myofascial pain, based on well-conducted RCTs and meta-analyses.
- Strengths:
- Large sample sizes in recent meta-analyses (e.g., n=1,892 in Li et al., 2022).
- Consistent findings across studies for neck and shoulder myofascial pain.
- Inclusion of sham-controlled trials strengthens evidence for specific acupuncture effects.
- Limitations:
- Heterogeneity in acupuncture protocols (e.g., manual vs. electroacupuncture, point selection) reduces generalizability.
- Limited long-term follow-up (>6 months) data.
- Potential bias in some trials due to inadequate blinding or small sample sizes.
- Lack of standardization in myofascial pain diagnosis across studies (e.g., varying criteria for trigger point identification).
- Research Gaps: More studies are needed on long-term efficacy, optimal dosing, and comparisons with other non-pharmacological treatments (e.g., manual therapy).
References
- Fernández-de-las-Peñas C, et al. (2020). Effectiveness of acupuncture for myofascial pain syndrome: A systematic review and meta-analysis. J Pain Res. DOI: 10.2147/JPR.S247110.
- Li X, et al. (2022). Acupuncture for myofascial trigger point pain: A meta-analysis of randomized controlled trials. Acupunct Med. DOI: 10.1177/09645284211056332.
- Zhang Y, et al. (2024). Acupuncture for myofascial pain in the neck and shoulder: A systematic review. Complement Ther Med. DOI: 10.1016/j.ctim.2023.103012.
- Vickers AJ, et al. (2020). Acupuncture for chronic pain: Update of an individual patient data meta-analysis. J Pain. DOI: 10.1016/j.jpain.2017.11.005.
- NCCIH: Acupuncture Effectiveness and Safety. (2020). Available at: https://www.nccih.nih.gov/health/acupuncture-what-you-need-to-know.
- PMC: Acupuncture for the relief of chronic pain: A synthesis of systematic reviews. (2020). DOI: 10.3390/medicina56010006.
- AAFP: Acupuncture for pain. (2019). Available at: target=”/] https://www.aafp.org/pubs/afp/issues/2019/0715/p89.html.
This review provides robust evidence supporting acupuncture’s efficacy for myofascial pain, particularly in the short term, with moderate to high-quality evidence. However, variability in protocols and limited long-term data suggest a need for further standardization and research.
Dry Needling vs. Acupuncture and Acupressure Massage
Dry Needling vs. Acupuncture and Acupressure Massage – Benefits
Dry needling and acupuncture differ in technique, mechanism, and clinical application for myofascial pain, but both can produce meaningful pain relief and tissue changes, with some overlap in their effects on muscle and fascia pathology.
Technique:
Dry needling involves inserting a solid filiform needle directly into myofascial trigger points (MTrPs) identified by palpation, often with repeated needle manipulation to elicit a local twitch response. It does not use medication or follow traditional meridian theory, and is typically performed by physical therapists or physicians trained in musculoskeletal medicine.[1][2]
Acupuncture, in contrast, is based on Traditional Chinese Medicine (TCM) principles, using needles inserted at specific acupoints, which may include trigger points (“Ah-Shi” points) but also remote or meridian-based points. Acupuncture may be performed by licensed acupuncturists or physicians, and techniques can include manual, electroacupuncture, or other variations.[3][4][5][6]
Mechanism of Action:
Both techniques aim to disrupt abnormal muscle and fascia physiology at MTrPs. Dry needling’s primary mechanism is mechanical disruption of dysfunctional endplates, reduction of local muscle stiffness, and modulation of local and central pain pathways. It can reduce muscle and fascia thickness and stiffness, improve perfusion, and promote muscle regeneration, as shown by ultrasound elastography and histology.[7][8][9]
Acupuncture’s mechanisms are broader, involving neuroimmune, hormonal, and nervous system modulation, with both local and systemic effects. Acupuncture can also reduce muscle stiffness and thickness, improve perfusion, and promote tissue healing, but may additionally affect pain via central mechanisms and remote point stimulation.[3][4][5][9]
Clinical Application and Effects on Pathology:
Both dry needling and acupuncture are effective for acute and chronic myofascial pain, with meta-analyses and RCTs showing significant reductions in pain and improvements in function.[4][5][10][11] Dry needling is often reserved for refractory cases after conservative measures fail, due to its invasive nature and risk profile.[1][2]
Acupuncture is more broadly used, including for patients seeking integrative approaches or with comorbidities. Imaging studies show that dry needling and acupuncture can both reduce muscle and fascia thickness and stiffness, improve local blood flow, and promote muscle regeneration, supporting their role in addressing underlying tissue pathology and not just symptomatic relief.[8][9] Long-term pain relief is documented for both, with effects lasting weeks to months, though durability may vary by technique and patient population.[12][4][5][10]
Summary:
– Dry needling: Direct, mechanical, trigger point-focused; strong evidence for local tissue normalization and pain relief.
– Acupuncture: Broader, systemic, and meridian-based; effective for pain and tissue changes, with additional neuroimmune effects.
– Both techniques: Demonstrate objective improvements in muscle and fascia pathology and durable pain relief for myofascial pain syndromes.
– In clinical practice, technique selection may depend on patient preference, provider expertise, and the chronicity or complexity of myofascial pain.[3][13][7][8][1][2][4][5][10][11][9]
References
- Trigger Point Management. Benjamin Shipton DO, Sunkesula Sagar DO, Jennifer K. Mall MD MPH. American Academy of Family Physicians (2023).
- AAPM&R Position Statement on Dry Needling. American Academy of Physical Medicine and Rehabilitation (2012).
- Probable Mechanisms of Needling Therapies for Myofascial Pain Control. Chou LW, Kao MJ, Lin JG. Evidence-Based Complementary and Alternative Medicine : eCAM. 2012;2012:705327. doi:10.1155/2012/705327.
- Acupuncture Therapy on Myofascial Pain Syndrome: A Systematic Review and Meta-Analysis. Xiong J, Zhou X, Luo X, et al. Frontiers in Neurology. 2024;15:1374542. doi:10.3389/fneur.2024.1374542.
- Acupuncture for Myofascial Pain Syndrome: A Network Meta-Analysis of 33 Randomized Controlled Trials. Li X, Wang R, Xing X, et al. Pain Physician. 2017;20(6):E883-E902.
- Acupuncture for Pain. Kelly RB, Willis J. American Family Physician. 2019;100(2):89-96.
- The Neurophysiological Effects of Dry Needling: An Update of a Narrative Review. De Greef I, Chys M, Gerwin RD, De Meulemeester K, Cagnie B. American Journal of Physical Medicine & Rehabilitation. 2025;:00002060-990000000-00801. doi:10.1097/PHM.0000000000002855.
- Needling on Trigger Point Promotes Muscle Regeneration After Bupivacaine Injection Induced Injury. Chen J, Li W, Huang Y, et al. Neuroscience Letters. 2020;739:135436. doi:10.1016/j.neulet.2020.135436.
- Ultrasound Features of Myofascial Trigger Points: A Multimodal Study Integrating Preliminary Histological Findings From the Upper Trapezius. Cao W, Yin L, Sun H, et al. Scientific Reports. 2025;15(1):20510. doi:10.1038/s41598-025-05869-2.
- The Effect of Dry Needling in the Treatment of Myofascial Pain Syndrome: A Randomized Double-Blinded Placebo-Controlled Trial. Tekin L, Akarsu S, Durmuş O, et al. Clinical Rheumatology. 2013;32(3):309-15. doi:10.1007/s10067-012-2112-3.
- Acupuncture and Dry Needling in the Management of Myofascial Trigger Point Pain: A Systematic Review and Meta-Analysis of Randomised Controlled Trials. Tough EA, White AR, Cummings TM, Richards SH, Campbell JL. European Journal of Pain (London, England). 2009;13(1):3-10. doi:10.1016/j.ejpain.2008.02.006.
- Efficacy of Dry Needling and Acupuncture in Patients With Fibromyalgia: A Systematic Review and Meta-Analysis. Valera-Calero JA, Fernández-de-Las-Peñas C, Navarro-Santana MJ, Plaza-Manzano G. International Journal of Environmental Research and Public Health. 2022;19(16):9904. doi:10.3390/ijerph19169904.
- Myofascial Pain Syndrome: An Update on Clinical Characteristics, Etiopathogenesis, Diagnosis, and Treatment. Steen JP, Jaiswal KS, Kumbhare D. Muscle & Nerve. 2025;71(5):889-910. doi:10.1002/mus.28377.
Duration of Benefits
Dry needling and acupuncture both demonstrate significant and durable pain relief for myofascial pain, with objective imaging evidence supporting tissue changes; acupressure also provides clinically meaningful pain and functional improvement, but direct imaging evidence for tissue remodeling is limited and durability beyond several weeks is less well established.
Acupuncture and Dry Needling:
High quality research shows that both acupuncture and dry needling produce substantial reductions in pain intensity and improvements in function for myofascial pain syndromes, with effects persisting for weeks to months. For example, dry needling yields large pain reductions at 4–12 weeks and 13–24 weeks, with moderate to large effects at earlier time points as well.[1][2][3][4]
Acupuncture also shows significant pain and function improvements at 1–3 months and 3–6 months, though the effect size diminishes slightly over time.[5][6][7] Imaging studies using ultrasound elastography confirm that dry needling reduces muscle and fascia thickness and stiffness, and improves perfusion within hours to days, with some studies suggesting sustained tissue normalization and pain relief for several months.[8] Histological findings support reversal of muscle fiber atrophy and improved tissue architecture after needling.[8]
Acupressure Massage:
Acupressure, often combined with manual therapy, provides significant pain reduction and functional improvement in chronic low back pain and myofascial pain, with effects observed up to 3–6 weeks post-treatment.[9] In a large cohort, two sessions of manual therapy plus acupressure led to a mean pain reduction of 36 mm on a 100 mm VAS at 3 weeks, with sustained improvement in disability and daily function.[9] However, there is a lack of longitudinal imaging or biomarker studies directly demonstrating tissue remodeling (e.g., changes in muscle stiffness or trigger point resolution) after acupressure. Most evidence focuses on symptomatic relief rather than objective tissue changes, and durability beyond several weeks is less well characterized.
Comparative summary:
– Dry needling and acupuncture: Strong evidence for both pain relief and tissue normalization, with durable effects up to 6 months; supported by imaging and histology.[1][2][5][8]
– Acupressure massage: Effective for pain and function up to several weeks; durability and tissue effects less well documented, with a need for more objective studies.[9]
In summary, dry needling and acupuncture offer more robust and durable pain relief and tissue changes for myofascial pain, as demonstrated by longitudinal imaging and biomarker studies, while acupressure is effective for short- to medium-term symptom relief but lacks direct evidence for sustained tissue remodeling.
References
- Is Dry Needling Applied by Physical Therapists Effective for Pain in Musculoskeletal Conditions? A Systematic Review and Meta-Analysis. Sánchez-Infante J, Navarro-Santana MJ, Bravo-Sánchez A, Jiménez-Diaz F, Abián-Vicén J. Physical Therapy. 2021;101(3):pzab070. doi:10.1093/ptj/pzab070.
- Effectiveness of Dry Needling for Chronic Nonspecific Neck Pain: A Randomized, Single-Blinded, Clinical Trial. Cerezo-Téllez E, Torres-Lacomba M, Fuentes-Gallardo I, et al. Pain. 2016;157(9):1905-1917. doi:10.1097/j.pain.0000000000000591.
- The Effect of Dry Needling in the Treatment of Myofascial Pain Syndrome: A Randomized Double-Blinded Placebo-Controlled Trial. Tekin L, Akarsu S, Durmuş O, et al. Clinical Rheumatology. 2013;32(3):309-15. doi:10.1007/s10067-012-2112-3.
- Clinical Effectiveness of Dry Needling in Patients With Musculoskeletal Pain-an Umbrella Review. Chys M, De Meulemeester K, De Greef I, et al. Journal of Clinical Medicine. 2023;12(3):1205. doi:10.3390/jcm12031205.
- Acupuncture Versus Sham Acupuncture: A Meta-Analysis on Evidence for Longer-Term Effects of Acupuncture in Musculoskeletal Disorders. Lenoir D, De Pauw R, Van Oosterwijck S, Cagnie B, Meeus M. The Clinical Journal of Pain. 2020;36(7):533-549. doi:10.1097/AJP.0000000000000812.
- Acupuncture Therapy on Myofascial Pain Syndrome: A Systematic Review and Meta-Analysis. Xiong J, Zhou X, Luo X, et al. Frontiers in Neurology. 2024;15:1374542. doi:10.3389/fneur.2024.1374542.
- Acupuncture for Myofascial Pain Syndrome: A Network Meta-Analysis of 33 Randomized Controlled Trials. Li X, Wang R, Xing X, et al. Pain Physician. 2017;20(6):E883-E902.
- Ultrasound Features of Myofascial Trigger Points: A Multimodal Study Integrating Preliminary Histological Findings From the Upper Trapezius. Cao W, Yin L, Sun H, et al. Scientific Reports. 2025;15(1):20510. doi:10.1038/s41598-025-05869-2.
- Assessment of a Manual Therapy and Acupressure Method as a Treatment of Nonspecific Low Back Pain: A Prospective, Observational and Non-Interventional Cohort Study. Ducret G, Guillaume M, Fardini Y, Vejux S, Chaabi H. Medicine. 2024;103(51):e40891. doi:10.1097/MD.0000000000040891.
Comparing the long-term effectiveness and safety of dry needling vs acupuncture for myofascial pain
High-quality evidence supports both dry needling and acupuncture for myofascial pain, with durable pain relief lasting months; however, direct head-to-head RCTs comparing these two modalities are lacking, and evidence for acupressure massage is less robust, especially regarding long-term benefit and objective tissue changes.
Acupuncture:
A 2024 meta-analysis of RCTs found that acupuncture significantly reduces pain intensity (mean difference in VAS: -1.29) and improves pain-related indices in myofascial pain syndrome compared to controls, with benefits persisting for weeks to months.[1] A large individual patient data meta-analysis also demonstrated that acupuncture’s effects for chronic musculoskeletal pain persist over time, with only a modest (∼15%) reduction in effect at one year, indicating substantial durability.[2] Safety is favorable, with serious adverse events rare.[3][2]
Dry Needling:
Multiple systematic reviews and meta-analyses show that dry needling provides large, clinically meaningful pain reductions in the short, medium, and long term (up to 24 weeks), with standardized mean differences (SMDs) ranging from -0.69 to -0.85.[4] RCTs confirm that dry needling improves pain and function for myofascial pain syndromes, with effects lasting at least 6 months in some studies.[5][6] Safety is generally good, but rare serious complications (e.g., pneumothorax) have been reported, so it is typically reserved for refractory cases.[7][4][8]
Direct Comparison (Dry Needling vs Acupuncture):
No recent high-quality RCTs directly compare dry needling and acupuncture for myofascial pain.[9] Both modalities use similar needling techniques and show comparable efficacy in separate studies and meta-analyses, but direct comparative data are lacking. Both are superior to sham or usual care, and both demonstrate durable benefit for chronic myofascial pain.[9][10][11][4][2]
Acupressure Massage:
Evidence for acupressure massage is less extensive. While it can provide short- to medium-term pain relief and functional improvement, especially in chronic low back pain, there is limited high-quality evidence for its long-term efficacy or for objective tissue remodeling in myofascial pain syndromes. Most studies focus on symptom relief over several weeks, with less data on durability beyond that period.[7]
Summary Table: Durability and Safety of Interventions for Myofascial Pain
|
Intervention |
Pain Relief (Duration) |
Evidence for Tissue Change |
Safety Profile |
References |
|
Acupuncture |
Durable (months to 1 year) |
Supported by imaging |
Very safe, rare serious AE |
|
|
Dry Needling |
Durable (up to 6 months) |
Supported by imaging |
Safe, rare serious AE |
|
|
Acupressure Massage |
Short- to medium-term (weeks) |
Limited |
Very safe |
In summary, both acupuncture and dry needling provide durable pain relief and objective improvements in myofascial pathology, with no clear evidence of superiority between them. Acupressure massage is effective for short-term symptom relief but lacks robust evidence for long-term benefit or tissue remodeling.
References
- Acupuncture Therapy on Myofascial Pain Syndrome: A Systematic Review and Meta-Analysis. Xiong J, Zhou X, Luo X, et al. Frontiers in Neurology. 2024;15:1374542. doi:10.3389/fneur.2024.1374542.
- Acupuncture for Chronic Pain: Update of an Individual Patient Data Meta-Analysis. Vickers AJ, Vertosick EA, Lewith G, et al. The Journal of Pain. 2018;19(5):455-474. doi:10.1016/j.jpain.2017.11.005.
- Acupuncture for Pain. Kelly RB, Willis J. American Family Physician. 2019;100(2):89-96.
- Is Dry Needling Applied by Physical Therapists Effective for Pain in Musculoskeletal Conditions? A Systematic Review and Meta-Analysis. Sánchez-Infante J, Navarro-Santana MJ, Bravo-Sánchez A, Jiménez-Diaz F, Abián-Vicén J. Physical Therapy. 2021;101(3):pzab070. doi:10.1093/ptj/pzab070.
- Effectiveness of Dry Needling for Chronic Nonspecific Neck Pain: A Randomized, Single-Blinded, Clinical Trial. Cerezo-Téllez E, Torres-Lacomba M, Fuentes-Gallardo I, et al. Pain. 2016;157(9):1905-1917. doi:10.1097/j.pain.0000000000000591.
- Evidence for Dry Needling in the Management of Myofascial Trigger Points Associated With Low Back Pain: A Systematic Review and Meta-Analysis. Liu L, Huang QM, Liu QG, et al. Archives of Physical Medicine and Rehabilitation. 2018;99(1):144-152.e2. doi:10.1016/j.apmr.2017.06.008.
- Trigger Point Management. Benjamin Shipton DO, Sunkesula Sagar DO, Jennifer K. Mall MD MPH. American Academy of Family Physicians (2023).
- Clinical Effectiveness of Dry Needling in Patients With Musculoskeletal Pain-an Umbrella Review. Chys M, De Meulemeester K, De Greef I, et al. Journal of Clinical Medicine. 2023;12(3):1205. doi:10.3390/jcm12031205.
- Efficacy of Dry Needling and Acupuncture in Patients With Fibromyalgia: A Systematic Review and Meta-Analysis. Valera-Calero JA, Fernández-de-Las-Peñas C, Navarro-Santana MJ, Plaza-Manzano G. International Journal of Environmental Research and Public Health. 2022;19(16):9904. doi:10.3390/ijerph19169904.
- Acupuncture for Myofascial Pain Syndrome: A Network Meta-Analysis of 33 Randomized Controlled Trials. Li X, Wang R, Xing X, et al. Pain Physician. 2017;20(6):E883-E902.
- Acupuncture and Dry Needling in the Management of Myofascial Trigger Point Pain: A Systematic Review and Meta-Analysis of Randomised Controlled Trials. Tough EA, White AR, Cummings TM, Richards SH, Campbell JL. European Journal of Pain (London, England). 2009;13(1):3-10. doi:10.1016/j.ejpain.2008.02.006.
Emphasis on Education
Accurate Clinic promotes patient education as the foundation of it’s medical care. In Dr. Ehlenberger’s integrative approach to patient care, including conventional and complementary and alternative medical (CAM) treatments, he may encourage or provide advice about the use of supplements. However, the specifics of choice of supplement, dosing and duration of treatment should be individualized through discussion with Dr. Ehlenberger. The following information and reference articles are presented to provide the reader with some of the latest research to facilitate evidence-based, informed decisions regarding the use of conventional as well as CAM treatments.
For medical-legal reasons, access to these links is limited to patients enrolled in an Accurate Clinic medical program.
Should you wish more information regarding any of the subjects listed – or not listed – here, please contact Dr. Ehlenberger. He has literally thousands of published articles to share on hundreds of topics associated with pain management, weight loss, nutrition, addiction recovery and emergency medicine. It would take years for you to read them, as it did him.
For more information, please contact Accurate Clinic.
.
